Meningitis
What causes meningitis?
Meningitis refers to inflammation of the membranes that cover the brain and spinal cord. The outer membrane is known as the meninges; meningitis, therefore is defined as inflammation of the meninges.
Meningitis can be caused by a number of infections, including bacterial, viral, fungal, and protozoal infections. These infections may reach the central nervous system via the sinuses, the inner ear, the vertebrae, or traumatic injuries. In some cases, infections may reach the central nervous system via the bloodstream.
Meningitis may also be non-infectious in nature, caused by an immune-mediated inflammatory response (in which the body’s immune system attacks its own tissues).
Additionally, some parasites may migrate through the brain and central nervous tissues, causing meningitis. Baylisascaris procyonis (a roundworm of raccoons) and heartworms are both known to cause parasitic meningitis in rare cases.
In cats, the most common causes of meningitis include feline infectious peritonitis (FIP), cryptococcosis, and toxoplasmosis.
In dogs, meningitis is rare but is most commonly diagnosed in Beagles, Bernese Mountain dogs, and Germain shorthaired Pointers. There is no age or sex predisposition. The most common type in dogs is steroid-responsive meningitis (also known as steroid-responsive meningitis-arteritis). This immune-mediated condition is most commonly seen during early adulthood.

What are the clinical signs of meningitis?
Common clinical signs of meningitis include fever, generalized pain (which may be severe), and rigidity of the neck. Affected pets are often lethargic and may refuse to eat.
Although meningitis itself does not cause neurologic signs, it may occur in association with encephalitis (inflammation of the brain), in a condition called meningoencephalitis. Pets with meningoencephalitis may show neurologic signs, including seizures, depression, paralysis, blindness, pacing, circling, and loss of consciousness.
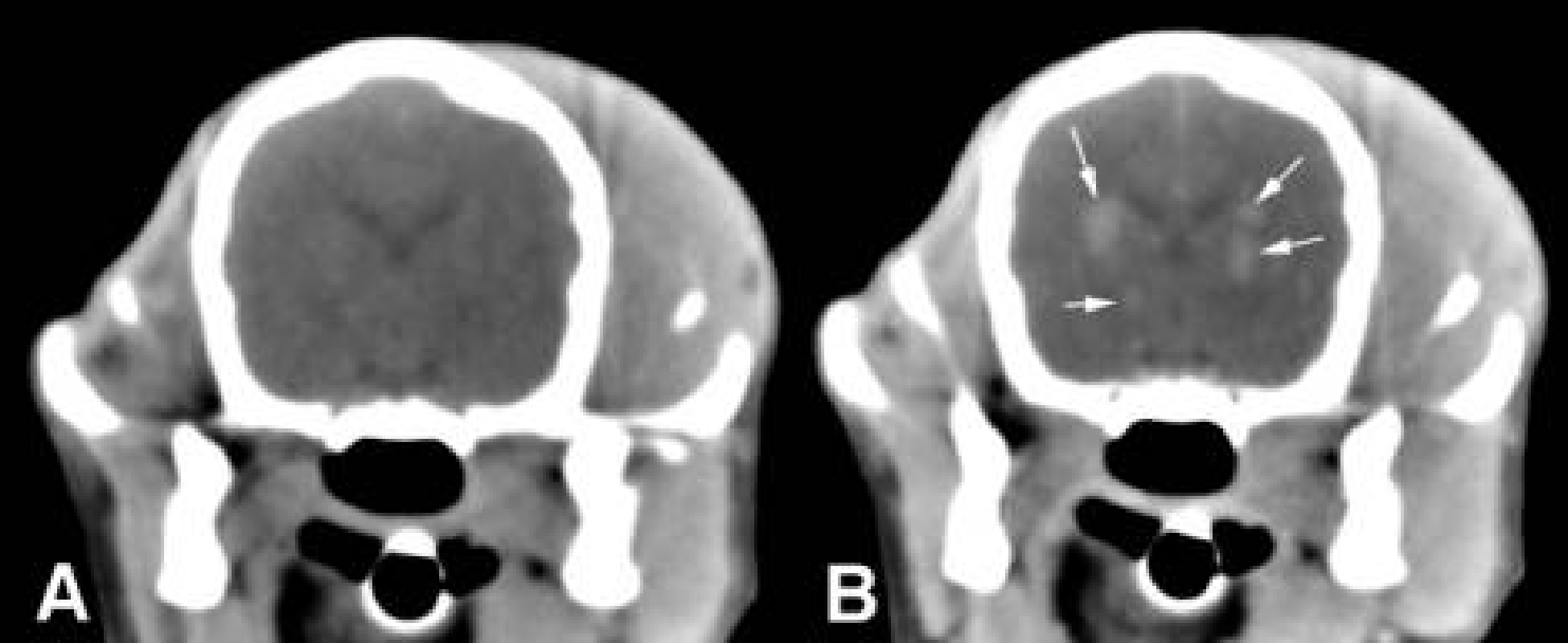
How will my veterinarian diagnose meningitis?
Your veterinarian will begin by performing a thorough physical exam on your pet. Signs that may suggest meningitis include neck pain, decreased blood pressure, and changes to the optic nerve that may be visible on ophthalmic (eye) exam.
Next, your veterinarian will likely perform complete baseline laboratory tests, including a complete blood cell count (CBC), serum biochemistry profile, and urinalysis. These tests will provide important information about your pet’s overall health and may provide an alternative explanation for your pet’s signs of illness.
If your pet’s bloodwork is normal, additional (more specialized) testing will likely be recommended. In many cases, your pet may be referred to a neurologist for these tests.
The most important diagnostic test in meningitis is a cerebrospinal fluid (CSF) tap. For this test, your pet is placed under general anesthesia. A needle is then inserted between the vertebrae in your pet’s neck or lower back, allowing your veterinarian to collect a small amount of the CSF fluid that bathes the brain and spinal cord. This fluid is analyzed for the presence of abnormal protein levels, inflammatory cells, infectious organisms, or other indicators of disease. In many cases, analyzing the CSF fluid can not only diagnose meningitis, but also suggest an underlying cause.
Your veterinarian may also recommend magnetic resonance imaging (MRI) or computed tomography (CT) of the brain. These tests are often performed during the same anesthetic episode as the CSF tap. Imaging with MRI or CT scan can provide additional information about the brain and meninges.
How is meningitis treated?
The treatment of meningitis depends largely on the underlying cause. In most cases, pets are critically ill when they present to the veterinarian and require hospitalization for aggressive treatment. Your veterinarian will perform frequent neurologic examinations on your pet during the course of treatment, in order to assess how he/she is responding to therapy.
Bacterial and protozoal infections are typically treated with antibiotics. In some cases, your veterinarian may begin with a broad-spectrum antibiotic and then change medications based on the results of CSF culture and sensitivity (a test in which bacteria are isolated from the CSF and tested to determine which antibiotics are most effective against the bacteria that are present).
Steroid-responsive meningitis is typically treated with prednisone. Pets are initially started on a relatively high dose of prednisone, with the dose tapered over the first several weeks of treatment. Side effects of prednisone treatment include increased thirst and urination, increased appetite, and increased susceptibility to infection. Long-term prednisone treatment (up to a year or more) may be required to prevent relapse.
Viral meningitis does not have a medical cure; it is treated with supportive care. Supportive care measures that may be used in viral meningitis, as well as in other cases of meningitis, include intravenous fluids to keep your pet hydrated, medications to decrease brain swelling, pain medications to alleviate discomfort, and nursing care.